
How can the NHS use data and artificial intelligence (AI)?
With the emergence of artificial intelligence (AI), Dick Wall (Healthcare BI Solutions Architect) discusses how NHS and healthcare providers can address real issues using the data at their fingertips.
AI is seen as the magic new development of computers, especially for the NHS and its rich data sources. If you believe the news, then it’ll end up putting all sorts of knowledge workers out of work as computers learn to do a variety of tasks previously reserved for humans.
But will Alexa really diagnose you and give you a prescription any time soon?
Here is an example from an advanced Trust looking at improving missed appointments. The truth is more complex and quite different. AI is a powerful tool but not yet a magic wand. Is it another useful tool that requires judgment, it’s not the ‘fix all’ promised by sections of the press? AI can be really powerful, but results need changes in operational and clinical approaches but depends upon teamwork and collaboration.
Our increasing volume and granularity of data as well as our growing analytics capability means we are able to start using our data in more innovative ways…
Eghosa Bazuaye
Our increasing volume and granularity of data as well as our growing analytics capability means we are able to start using our data in more innovative ways…
Eghosa Bazuaye
Real-world NHS Data and AI examples
During a recent discussion with Eghosa Bazuaye, the Associate Director of Informatics at Royal Berkshire NHS Trust (RBH), one of the first trusts to adopt the Bedrock Data Warehouse and the real-time connector. RBH is on a journey to collect, and curate data and use it to change the course of events, not just report on them. They use the Bedrock platform to get real-time data from their Electronic Patient Record. This allows them to curate and use all of their data in a few seconds after it has been added to the system.
The trust is on a journey from doing the minimum reporting with messy data to supporting clinicians and managers with accurate real-time data that helps them predict and so change outcomes. This project is one of many that take advantage of copious volumes of clean data delivered in real-time by Bedrock.
Solving the ‘Patient Did Not Attend’ mysteries
Did Not Attend (DNA) is a significant issue to the UK. The “free at the point of delivery” model that is key to the NHS means that someone not attending an outpatient appointment is an irrecoverable loss of the resources needed to run a clinic.
In RBH, the overall DNA rate is about 7% at a probable cost to the Trust of about £3m a year, not including the lost opportunity to see other patients.
The DNA project used the ready supply of data held in Bedrock to look for patterns in the properties of appointments that were not attended. With a large, high-quality data set there are many possibilities. Humans can use all manner of slicing and dicing to look over the data and come up with explanations for DNAs. Talking to NHS teams there are no end of explanations (urban myths?) that have arisen over the years. Age, sex, geography and time of appointment are known to affect DNA.
The stereotypes say that a 63-year-old woman will attend any appointment, but a 19-year-old man is less likely to attend anything but a Wednesday afternoon. And people also throw in explanations like public transport, demographics, working patterns and other issues. In our research at Trustmarque, we have also seen just plain wrong booking systems that don’t allow a patient to say they can’t attend so don’t discount the sample.
The AI alternative is to use Machine Learning to look at a large set of historical data and to look for patterns in the properties of DNAs and appointments. That was the approach at RBH.
The DNA issues at RBH used an AI approach that produce and probability score data from the Bedrock Platform that can were then split into two groups. First was “here are a few appointments that are very likely to be missed” and a second group of many more appointments that are less likely – but still quite likely to be missed.
The first was higher precision and the second was higher recall. Briefly explained higher precision only selected a subset of proposed appointments that were very likely to ‘DNA’. But it would exclude many that were quite likely to ‘DNA’. The Higher Recall result gave a larger volume of predicted DNAs, but was less discriminating.
Did it work? Yes – but the answer was also “It’s complicated”. In this case the AI could find a small number of more likely (>75%) to DNA (a few higher precision predictions) and larger number of quite probable predictions (higher recall). This was no magic solution but, a lot more information.
“This is an illustration of the realities of using your data. RBH are successful in getting real benefit from data by integrating clinical, operational and data resources to address an organisational problem. By discussing the issues as a team and thinking through practical and effective approaches that can work.”
Dick Wall (Healthcare BI Solutions Architect)
Driving change with AI
So, did AI solve all the problems? Well, not just AI – it needed the AI to drive changes in what the clinical and operational teams do. What the project did was present a different way of looking at the problem. They then have had to look at how to operationally respond to these findings.
For instance, if you are very confident that an appointment is very likely to be missed, you may well be willing to invest more resources on avoiding that. You have choices; you might choose to offer transport for the highly likely ones if you think that transport is the issue. There are a range of other responses, offering appointments less likely to DNA, sending automated text reminders, calls and asking if they are attending. And the local University were able to bring some psychological insights to draft the targeted texts to send to the people in different groups, and then use the tool to send the right messages! Of course, all of the predicted scores and actions taken were captured and sent to the Bedrock Data Warehouse for further analysis.
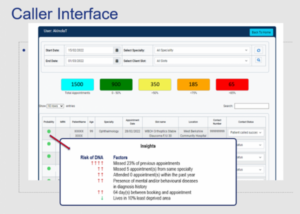
The pilot details are interim but achieved a five-fold reduction in the proportion of DNAs by using the AI driven contact approach
So, will Alexa be writing prescriptions? Probably not for the foreseeable future, but data and AI are showing how the NHS can address real issues using the data that they already have.
About the author
Dick Wall started in IT in 1987 before the PC or MS-Dos and has always been interested in how IT delivers (or doesn’t) value to the organisation using it. He now works almost exclusively with the NHS to help them deliver clinical and operational value from the data collected in many disparate digital systems that touch patients and staff.
Working closely with Healthcare organisations across the UK, Dick supports the development of Business Intelligence (BI) solutions to facilitate improvements in operational, commercial, financial and resource challenges using data and information as an enabler in the process.



